Search
- Page Path
- HOME > Search
Original Article
- Use of doxorubicin-eluting bead transarterial chemoembolization for unresectable hepatocellular carcinoma with portal vein invasion: a prospective study
- Su Jong Yu, Yun Bin Lee, Eun Ju Cho, Jeong-Hoon Lee, Hyo-Cheol Kim, Jin Wook Chung, Jung-Hwan Yoon, Yoon Jun Kim
- J Liver Cancer. 2023;23(1):166-176. Published online March 3, 2023
- DOI: https://doi.org/10.17998/jlc.2023.02.08
- 2,794 Views
- 117 Downloads
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material - Background/Aim
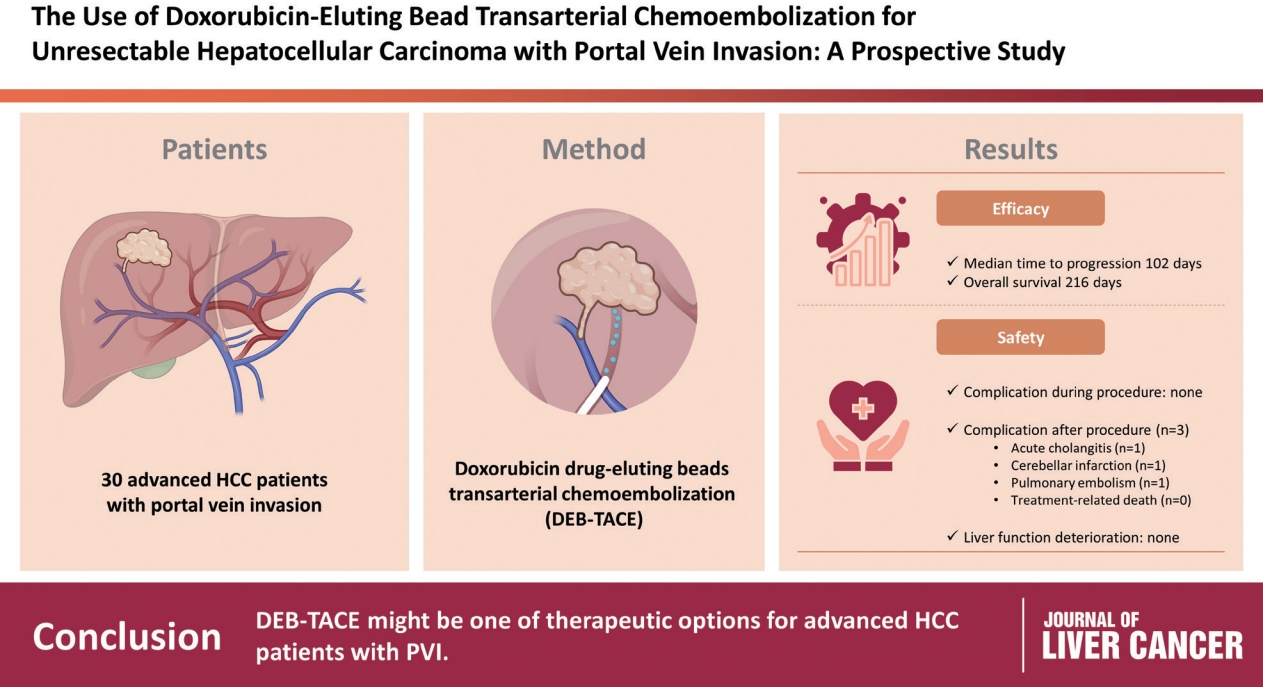
To evaluate the applicability of transarterial chemoembolization (TACE) treatment with doxorubicin drug-eluting beads (DEBs) in advanced hepatocellular carcinoma (HCC) patients with portal vein invasion (PVI).
Methods
This prospective study was approved by the institutional review board and informed consent was obtained from all participants. A total of 30 HCC patients with PVI received DEB-TACE between 2015 and 2018. The following parameters were evaluated: complications during DEB-TACE, abdominal pain, fever, and laboratory outcomes, including liver function change. Overall survival (OS), time to progression (TTP), and adverse events were also analyzed and assessed.
Results
DEBs measuring 100–300 μm in diameter were loaded with doxorubicin (150 mg per procedure). There were no complications during DEB-TACE and no significant differences in the levels of prothrombin time, serum albumin, or total bilirubin at follow-up compared to baseline. The median TTP was 102 days (95% confidence interval [CI], 42–207 days) and the median OS was 216 days (95% CI, 160–336 days). Three patients (10%) had severe adverse reactions, including transient acute cholangitis (n=1), cerebellar infarction (n=1), and pulmonary embolism (n=1), but no treatment-related death occurred.
Conclusions
DEB-TACE may be a therapeutic option for advanced HCC patients with PVI.

Review Article
- Radioembolization for hepatocellular carcinoma: what clinicians need to know
- Jin Woo Choi, Hyo-Cheol Kim
- J Liver Cancer. 2022;22(1):4-13. Published online February 23, 2022
- DOI: https://doi.org/10.17998/jlc.2022.01.16

- 9,477 Views
- 491 Downloads
- 9 Citations
-
 Abstract
Abstract
 PDF
PDF - Transarterial radioembolization (TARE) with yttrium 90 (90Y) has been used in the management of hepatocellular carcinoma (HCC) for more than 10 years in Korea. There are two types of 90Y radioactive microspheres available, namely, glass and resin microspheres, with comparable clinical outcomes. In general, TARE outperforms transarterial chemoembolization regarding post-embolization syndrome, time to progression, tumor downsizing for liver transplantation, and hospitalization stay. Although TARE is commonly recommended for patients with unresectable large HCCs, it can be an alternative to or performed in combination with ablation, surgical resection, and systemic treatment. This review aimed to address 90Y radioactive microspheres, patient selection, clinical outcomes, simulation tests, radioembolization procedures, follow-up imaging, and complications.
-
Citations
Citations to this article as recorded by- Unlocking Precision in Radioembolization: Navigating the Future of Holmium-166 Radioembolization Mapping and Lung Shunt Study by Implementing Scout Dosimetry
Peiman Habibollahi, Armeen Mahvash, Nima Kokabi, Nariman Nezami
CardioVascular and Interventional Radiology.2024; 47(4): 451. CrossRef - Feasibility of Liver Transplantation after 90Y Radioembolization: Lessons from a Radiation Protection Incident
Marine Soret, Jacques-Antoine Maisonobe, Philippe Maksud, Stéphane Payen, Manon Allaire, Eric Savier, Charles Roux, Charlotte Lussey-Lepoutre, Aurélie Kas
Health Physics.2024; 127(3): 373. CrossRef - Liver-Directed Locoregional Therapies for Neuroendocrine Liver Metastases: Recent Advances and Management
Cody R. Criss, Mina S. Makary
Current Oncology.2024; 31(4): 2076. CrossRef - Selective internal radiation therapy segmentectomy: A new minimally invasive curative option for primary liver malignancies?
Riccardo Inchingolo, Francesco Cortese, Antonio Rosario Pisani, Fabrizio Acquafredda, Roberto Calbi, Riccardo Memeo, Fotis Anagnostopoulos, Stavros Spiliopoulos
World Journal of Gastroenterology.2024; 30(18): 2379. CrossRef - Transarterial chemoembolization as an alternative to radioembolization is associated with earlier tumor recurrence than in radioembolization-eligible patients
Sung Won Chung, Heejin Cho, Hyunjae Shin, Jeayeon Park, Ju Yeon Kim, Ji Hoon Hong, Moon Haeng Hur, Min Kyung Park, Yun Bin Lee, Su Jong Yu, Myungsu Lee, Yoon Jun Kim, Jin Chul Paeng, Jung-Hwan Yoon, Jin Wook Chung, Jeong-Hoon Lee, Hyo-Cheol Kim
Frontiers in Oncology.2023;[Epub] CrossRef - The evolution of immune checkpoint inhibitor combinations in advanced hepatocellular carcinoma – A systematic review
Brandon M. Meyers, Jennifer J. Knox, David M. Liu, Deanna McLeod, Ravi Ramjeesingh, Vincent C. Tam, Howard J. Lim
Cancer Treatment Reviews.2023; 118: 102584. CrossRef - Recent Advances in Image-Guided Locoregional Therapies for Primary Liver Tumors
Cody R. Criss, Mina S. Makary
Biology.2023; 12(7): 999. CrossRef - Multidisciplinary consensus recommendations for management of hepatocellular carcinoma in Middle East and North Africa region
Imam Waked, Sherif Alsammany, Sayed Hammad Tirmazy, Kakil Rasul, Jafar Bani‐Issa, Wael Abdel‐Razek, Ashraf Omar, Amr Shafik, Salem Eid, Amr Abdelaal, Ahmed Hosni, Gamal Esmat
Liver International.2023; 43(10): 2062. CrossRef - Impact of Low Skeletal Muscle Mass on Long-Term Outcomes in Hepatocellular Carcinoma Treated with Trans-Arterial Radioembolization: A Retrospective Multi-Center Study
Heechul Nam, Hyun Yang, Ho Soo Chun, Han Ah Lee, Joon Yeul Nam, Jeong Won Jang, Yeon Seok Seo, Do Young Kim, Yoon Jun Kim, Si Hyun Bae
Cancers.2023; 15(21): 5195. CrossRef
- Unlocking Precision in Radioembolization: Navigating the Future of Holmium-166 Radioembolization Mapping and Lung Shunt Study by Implementing Scout Dosimetry


 E-submission
E-submission THE KOREAN LIVER CANCER ASSOCIATION
THE KOREAN LIVER CANCER ASSOCIATION

 First
First Prev
Prev



 Follow JLC on Twitter
Follow JLC on Twitter