Articles
- Page Path
- HOME > J Liver Cancer > Volume 20(1); 2020 > Article
-
Review Article
Liver Magnetic Resonance Imaging for Hepatocellular Carcinoma Surveillance -
So Hyun Park1, Bohyun Kim2

-
Journal of Liver Cancer 2020;20(1):25-31.
DOI: https://doi.org/10.17998/jlc.20.1.25
Published online: March 31, 2020
1Department of Radiology, Gachon University Gil Medical Center, Gachon University College of Medicine, Incheon, Korea
2Department of Radiology, Seoul St. Mary’s Hospital, Seoul, Korea
-
Corresponding author : Bohyun Kim Department of Radiology, Seoul St. Mary’s Hospital, 222 Banpo-daero, Seocho-gu, Seoul 06591, Korea
Tel. +82-2-2258-5793, Fax. +82-2-599-6771 E-mail; kbh@cmcnu.or.kr
Copyright © 2020 The Korean Liver Cancer Association
This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/by-nc/4.0/) which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
- 5,572 Views
- 245 Downloads
- 5 Citations
Abstract
- Hepatocellular carcinoma (HCC) surveillance is recommended when the annual incidence of HCC exceeds 1.5%. In 2018, several international guidelines included alternative surveillance modalities, such as computed tomography and magnetic resonance imaging (MRI), as alternatives for patients with inadequate surveillance with an ultrasound. Currently, abbreviated MRI selectively includes several key sequences and is emerging as an effective tool for HCC surveillance with reduced cost and scan time and the required diagnostic performance. The incidence of HCC substantially impacts the benefits of surveillance in terms of cost-effectiveness. Therefore, we need to individualize imaging surveillance of HCC, tailor screening, and determine risk-stratified strategies. The purpose of this article was to present a brief overview of the diagnostic performance and cost-effectiveness of liver MRI as an HCC surveillance tool.
- Hepatocellular carcinoma (HCC) is the fifth most common type of cancer and a leading cause of cancer-related deaths worldwide [1,2]. It imposes a heavy annual economic burden that reached 454.9 million United States dollars from 1991 to 1999 [3]. The most common risk factor for HCC is liver cirrhosis caused by viral hepatitis, followed by alcoholic liver disease and nonalcoholic fatty liver disease [2]. To reasonably detect HCCs at an early and potentially curable stage, guidelines by the European Association for the Study of the Liver (EASL), American Association for the Study of Liver Diseases (AASLD), Asian Pacific Association for the Study of the Liver (APASL), and Korean Liver Cancer Association-National Cancer Center Korea (KLCA-NCC) currently recommend a surveillance program for HCC through biannual ultrasonography (US) with or without serum alpha fetoprotein (AFP) [1,4-6]. This strategy is largely supported by a randomized controlled trial in which biannual screening of patients with AFP and US resulted in a 37% decrease in mortality from HCC.7 Although US is an affordable and accessible modality for screening, meta-analyses reveal that it has an unsatisfactory 60-65% per-patient sensitivity for HCC detection in the cirrhotic liver,8,9 which is low for a screening test. The accuracy of US could further reduce in patients with obesity, advanced cirrhosis, or subcapsular lesions [10,11]. For HCCs smaller than 2 cm, the sensitivity of US is 20% or less [12-14]. Thus, failed or suboptimal US surveillance seems to contribute to an advanced-stage tumor presentation [15].
- Because detecting HCC at an early stage provides a wider range of options for curative treatments, a feasible and robust screening tool is required. To overcome limited efficacy of US, several guidelines updated in 2018 included alternative surveillance modalities, such as computed tomography (CT) or magnetic resonance imaging (MRI) in patients with inadequate US surveillance (Fig. 1) [1,4,6]. The purpose of this review was to present an overview of the diagnostic performance and cost-effectiveness of liver MRI as an HCC surveillance tool.
INTRODUCTION
- 1. Full-protocol gadoxetic acid-enhanced liver MRI: diagnostic performance
- Gadoxetic acid (Primovist or Eovist, Bayer Schering Parma, Berlin, Germany) is a gadolinium-based, hepatocytespecific MRI contrast agent that provides dynamic enhancement profile of the focal lesion as well as functional and structural information of the hepatobiliary system. Unlike conventional extracellular contrast media (ECCM), which only distributes in the extracellular space, gadoxetic acid enters the functioning hepatocyte and is then excreted into the biliary system approximately 20 minutes after injection [16]. T1-weighted imaging obtained in this specific temporal window is referred to as the hepatobiliary phase (HBP). On images obtained in HBP, most malignant focal liver lesions, including HCC, are hypointense compared to the strongly enhancing liver parenchyma, increasing the sensitivity for detecting such nodules [17]. Additionally, T1-weighted dual gradientecho in-phase and out-of-phase image (Dual-GRE), T2-weighted image (T2WI) and diffusion-weighted image (DWI) are obtained as part of the full-protocol liver MRI to preserve both the specificity and sensitivity for the diagnosis of HCC [17]. A meta-analysis revealed that gadoxetic acid-enhanced liver MRI was superior to dynamic contrast-enhanced CT or MRI using other types of ECCM and hepatocyte-specific contrast agents for detecting and characterizing liver lesions during the intrahepatic staging workup of HCC [18]. Owing to the high sensitivity and superior tissue contrast, gadoxetic acid-enhanced MRI could be a potential screening tool for HCCs. Kim et al. hypothesized that gadoxetic acid-enhanced MRI would show a significantly higher sensitivity compared to US for the detection of early-stage HCC in patients with cirrhosis at high risk of developing HCC [11]. Of the 423 patients at risk, 48 HCCs were diagnosed in 43 patients during 1,057 screening rounds using paired US and MRI at 6-month intervals, with most HCCs belonging to a very early stage or an early stage according to the Barcelona Clinic Liver Cancer (BCLC) staging system. The overall HCC detection rates of US and MRI were 27.9% and 86.0%, respectively. The false-positive rate was 5.6% (59/1,057) for US and 3.0% (32/1,057) for MRI, showing a notable difference. This study highlights the superior performance of gadoxetic acid-enhanced MRI compared to US in detecting very-earlystage HCCs in patients at a high risk for HCC, which in turn is associated with a higher probability of curative treatment and patient survival. However, the cost of gadoxetic acid-enhanced MRI is high, and concerns regarding how cost-effective this surveillance scheme is should be considered. The issue of cost-effectiveness will be addressed later in this article.
- 2. Abbreviated liver MRI (AMRI): suggested sequences and diagnostic performances
- AMRI is a shortened version of the full-sequence dynamic contrast-enhanced MRI, and is emerging as a practical screening modality for HCC. Advantages of AMRI are reduced scan time and cost in addition to an acceptable diagnostic performance, which are achieved by selectively including several key sequences. AMRI can be primarily divided into three categories (Table 1): noncontrast AMRI, HBP added to noncontrast AMRI (EOB-AMRI), and dynamic AMRI using an ECCM [19-23]. In prior studies, two to five key sequences were selected for each AMRI protocol to yield a fairly high per-patient sensitivity of 80-89.6% for the diagnosis of HCC [19-24]. Particularly, for noncontrast AMRI, the perpatient sensitivity and specificity ranged from 82.9-89.6% and 76.4-87.5%, respectively [21,23]. For EOB-AMRI, the sensitivity and specificity ranged from 80.6-83.7% and 90.6-91.6%, respectively [19,22]. Although these were heterogeneous studies carried out at different centers, all showed promising results for AMRI as a screening tool for HCC.
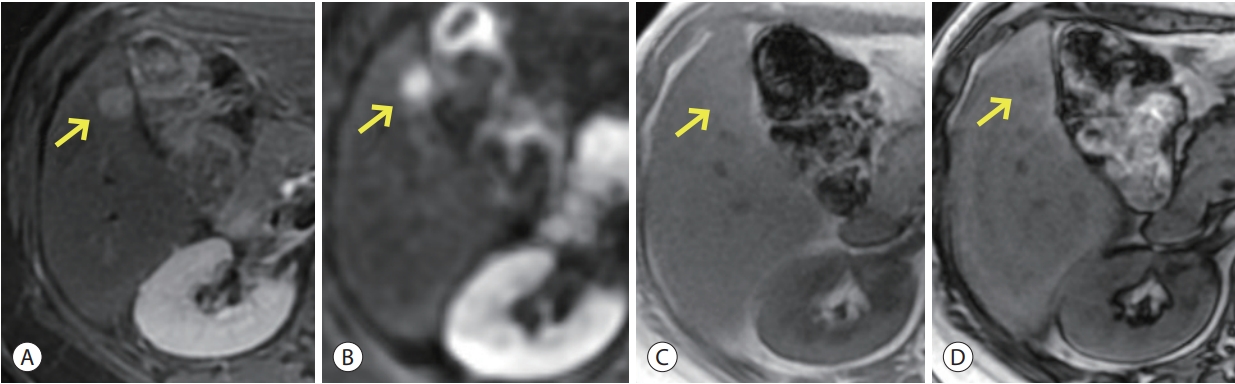
- Noncontrast AMRI was tested to detect HCC or other liver malignancies in several retrospective studies, mainly performed in South Korea (Fig. 2) [21,23,25]. Advantages of noncontrast AMRI are cheaper cost, safer study free of contrast agents, and simplicity in execution: If enough sequences are selected to preserve the sensitivity for HCC detection without the use of contrast agents, the risk of contrast agent-related adverse events is eliminated, and both the cost and examination time can be reduced. Han et al. found three effective key sequences: Half-Fourier Acquisition Single-shot Turbo spin Echo (HASTE) T2WI, Dual-GRE, and DWI [21]. During a reduced scan time of 12-15 minutes, the AMRI protocol showed per-patient sensitivities of 86.3% and 82.9% for HCC as evaluated by two independent readers. In the same study, per-lesion sensitivity ranged from 70.5-75.9% for detecting tumors within Milan criteria.
- There is an ongoing prospective, multicenter clinical trial evaluating the use of noncontrast AMRI as an HCC surveillance tool in patients with liver cirrhosis in South Korea [26]. The study aims to assess the detection rate of HCC using US at 6-months intervals compared to yearly noncontrast liver MRI over a 3-years follow-up [26]. In this trial, the AMRI protocol uses five sequences: HASTE T2WI, fast-spin-echo T2WI, Dual-GRE, DWI, and T1-weighted images. This trial might provide more solid evidence to support the utility of noncontrast MRI for HCC surveillance. Noncontrast AMRI has several great advantages as a surveillance tool for HCC; however, issues regarding sensitivity for detecting small lesions and its performance with a 1.5T system require further assessment. The prospective study might resolve some of these issues.
- EOB-AMRI for HCC surveillance has been evaluated in several retrospective studies mostly conducted in the United States of America [19,20,22]. These studies were designed to detect HCC greater than 1 cm using the tested sequences. The protocol is based on the hypothesis that AMRI consisting only of HBP and T2WI, essentially, and/or DWI could provide adequate per-patient sensitivity and negative predictive values for HCC surveillance. The rationale for the protocol was that most HCCs are hypointense in contrast to the liver parenchyma in HBP so that HCCs could be easily detected even in the absence of the dynamic contrast-enhanced studies. Additionally, T2WI in this protocol is useful in differentiating HCCs from cysts and hemangiomas showing a distinctively high T2 signal intensity. In EOB-AMRI, gadoxetic acid is hand-injected to the patient in the waiting room 20 minutes prior to the scan in order to save 20 minutes of time interval required to image HBP. If there is a suspicious lesion on EOB-AMRI, the patient is called back to undergo dynamic contrast-enhanced MRI. The main advantage of this protocol is its high sensitivity for detecting HCCs while remarkably reducing the scan time. Several studies have assessed the optimized sequence combination: Mark et al. found that the per-patient sensitivity of the T2WI sequence plus HBP did not improve even after adding DWI (82.6% vs. 83.7%) [19]. Besa et al. compared the sensitivity of HCC detection among several combinations of sequences, and per-patient sensitivity was reported to be 80.6% when T2WI, HBP, and DWI combination was used. The sensitivity was higher at 90.6% when dynamic contrast enhancement and T2WI were used [22]. Tillman et al. reported that the per-lesion sensitivity was 85.2% when the combination of T2WI and HBP was used [20]. Although the studies reported a satisfactory sensitivity, these were retrospective in nature and were based on simulated sets built from a full-sequence gadoxetic acid-enhanced MRI. Other unresolved issues are the need to optimize noncontrast sequences to balance the sensitivity, cost, and scan time. A high rate of false-positives should also be addressed. Additionally, the most effective confirmative dynamic contrastenhanced study of suspicious lesions detected on AMRI should be identified.
- A retrospective study using AMRI that only included dynamic enhancement using ECCM agents for HCC surveillance was conducted in the USA [24]. In this study, the AMRI protocol obtained pre-, arterial, portal, and 3-minutes-delayed phase images requiring approximately 7-10 minutes to perform. The authors compared AMRI utilizing only dynamic contrast-enhanced images to full-sequence liver MRI and reported that only 5% of cases would require modification in the Liver Imaging Reporting and Data System (LIRADS) category because of ancillary features on T2WI and DWI. The limitation of this study was its retrospective design based on a simulated set without a reference standard for the diagnosis of HCC. Advantages of dynamic AMRI are the short scan time, reduced cost, and ability to confirm the diagnosis.
LIVER MRI FOR HCC SURVEILLANCE
- The choice of a surveillance tool requires consideration of key factors, including the cost, sensitivity, and specificity for the disease, incidence of the disease, and increase in survival rates with the treatment [27-29]. HCC surveillance should be performed for patients whose risk for HCC development is high enough to make it cost-effective. Surveillance is considered effective if it increases the life expectancy by more than 3 months and cost-effective if 1 quality-adjusted life year is increased for less than $50,000 [30]. Therefore, the incidence of HCC is the primary determinant of cost-effectiveness of surveillance.
- The risk of developing HCC is not uniform across all patients even in the presence of risk factors. The annual risk of developing HCC ranges from 0.2% to over 10%. Therefore, it is necessary to stratify the risk and determine the target distribution. In patients with Child-Pugh A cirrhosis, HCC surveillance becomes cost-effective if the annual incidence of HCC exceeds 1.5% [31]. In patients with chronic hepatitis B without cirrhosis, surveillance is considered cost-effective if the incidence of HCC is greater than 0.2% [32]. When the incidence of HCC is greater than 3%, MRI surveillance is an acceptable, cost-effective option [33].
COST-EFFECTIVE ANALYSIS OF LIVER MRI FOR HCC SURVEILLANCE
- 1. Most effective confirmation study for an AMRI-detected lesion
- Because AMRI protocols are designed to detect suspicious lesions, further testing is required to confirm the diagnosis. Currently, the proposed scheme is to call the patients back for an additional dynamic contrast-enhanced study [19]. However, if the patient underwent a recent dynamic contrast-enhancement study, it may be a substitute and avoid a repeated scan. Park et al. reported that AMRI combined with recently performed multiphasic CT demonstrated a diagnostic performance similar or superior to a full-sequence gadoxetic acid-enhanced MRI for HCC using LI-RADS [34]. Therefore, in patients at risk for HCC, multiphasic CT could be potentially used as a sequential examination to confirm an AMRI-detected hepatic nodules.
- 2. Prospective comparison of the diagnostic capability of US and variable combinations of liver MRI sequences for HCC surveillance
- A prospective comparison of the diagnostic capability of US and other AMRI protocols should be performed because there have only been simulated retrospective studies so far. Many of these studies compared several different combinations of sequences to improve the sensitivity, but finding the best combination still requires further research. A recent study reported expected savings of up to 49% on a simulated cost-effective analysis when AMRI replaced full-sequence MRI [22]. This has been further emphasized in an estimated cost-effective analysis based on the medical cost of US: EOBAMRI was more cost-effective in patients at a high or intermediate risk for HCC [22]. A more detailed cost-effective analysis may provide evidence for tailored screening and a risk-stratified approach.
- 3. Role of serum markers combined with liver MRI for HCC surveillance
- Another consideration is to evaluate the possible benefit of combining serum marker results with AMRI findings.
- 4. Inter-reader agreement of liver MRI for HCC surveillance
- Inter- and intra-reader agreements should be validated since assessments could vary depending on the combination of sequences.
PERSPECTIVES ON FUTURE RESEARCH
- Several protocols of AMRI are under investigation to aid unsatisfactory performance of the currently recommended HCC surveillance using US. Yang et al. recently reported that the incidence of HCC and stage of progression of cirrhosis was associated with the strongest cost-effectiveness of surveillance [35], remarking that the incidence of HCC in the population and sensitivity of the surveillance tool substantially impact the benefits of HCC surveillance. Therefore, we need to individualize HCC surveillance through assessments of patients’ risk for HCC, diagnostic accuracy of the imaging tool, and costs of examinations.
CONCLUSION
-
The authors declare no conflicts of interest relevant to this article.
-
FINANCIAL DISCLOSURE
This study was supported by a research fund from the Scientific Research Fund of the Korean Liver Cancer Study Group.
Article information

| Study | No. of patients | No. of HCCs | Field strength | AMRI | MRI sequence | Per-patient sensitivity | Perpatient specificity | Inter-reader agreement |
|---|---|---|---|---|---|---|---|---|
| Kim et al. [25] | 135 | 116 | 3T | Noncontrast-AMRI | T2WI, Dual-GRE, and DWI | 91.7%* | 77.5% | k=0.615-0.733 |
| Han et al. [21] | 247 | 175 | 3T | Noncontrast-AMRI | T2WI, Dual-GRE, and DWI | 82.9-86.3% | 76.4-87.5% | k=0.668 |
| Kim et al. [23] | 226 | 173 | 3T | Noncontrast-AMRI | T2WI and DWI vs. T2WI, Dual-GRE, and DWI | 84.4-87.3% vs. 87.3-89.6% | 86.8 vs. 79.2-81.1% | k=0.77-0.78 |
| Marks et al. [19] | 298 | 49 | 1.5T | EOB-AMRI | T2WI and HBP vs. T2WI, HBP, and DWI | 82.6% vs 83.7% | 91.6% | k=0.72 |
| 3T | ||||||||
| Besa et al. [22] | 174 | 62 | 1.5T | EOB-AMRI | Various combinations using HBP and DWI vs. dynamic enhancement | 80.6%† | 90.6% | k=0.79-0.82 |
| 3T | ||||||||
| Tillman et al. [20] | 79 | 27 | 1.5T | EOB-AMRI | T2WI and HBP | 85.2%‡ | N/A | k=0.75 |
| 3T | ||||||||
| Lee et al. [24] | 164 | N/A | 3T | ECCM-AMRI | Pre-, arterial, portal, 3-min-delayed MRI (only dynamic phase AMRI) vs. full-sequence MRI | 5% of cases with changes in LI-RADs | N/A | k=0.508 |
HCC, hepatocellular carcinoma; AMRI, abbreviated magnetic resonance imaging; MRI, magnetic resonance imaging; T2WI, T2-weighted images; Dual-GRE, dual gradient-echo in-phase and out-of-phase image; DWI, diffusion-weighted imaging; EOB-AMRI, gadoxetic acid-enhanced AMRI; HBP, hepatobiliary phase; N/A, not available; ECCM-AMRI extracellular contrast media-enhanced AMRI; LI-RAD, Liver Imaging Reporting and Data System.
* Per-patient sensitivity for detection of malignancy;
† Sensitivities of DWI and HBP sequences;
‡ Per-lesion sensitivity for HCC.
- 1. European Association for the Study of the Liver. EASL Clinical Practice Guidelines: management of hepatocellular carcinoma. J Hepatol 2018;69:182−236.ArticlePubMed
- 2. Fattovich G, Stroffolini T, Zagni I, Donato F. Hepatocellular carcinoma in cirrhosis: incidence and risk factors. Gastroenterology 2004;127(5 Suppl 1): S35−S50.ArticlePubMed
- 3. Ghouri YA, Mian I, Rowe JH. Review of hepatocellular carcinoma: epidemiology, etiology, and carcinogenesis. J Carcinog 2017;16:1. ArticlePubMedPMC
- 4. Heimbach JK, Kulik LM, Finn RS, Sirlin CB, Abecassis MM, Roberts LR, et al. AASLD guidelines for the treatment of hepatocellular carcinoma. Hepatology 2018;67:358−380.ArticlePubMed
- 5. Omata M, Cheng AL, Kokudo N, Kudo M, Lee JM, Jia J, et al. Asia- Pacific clinical practice guidelines on the management of hepatocellular carcinoma: a 2017 update. Hepatol Int 2017;11:317−370.ArticlePubMedPMCPDF
- 6. Korean Liver Cancer Association. 2018 Korean Liver Cancer Association-National Cancer Center Korea Practice Guidelines for the management of hepatocellular carcinoma. Korean J Radiol 2019;20:1042−1113.ArticlePubMedPMC
- 7. Zhang BH, Yang BH, Tang ZY. Randomized controlled trial of screening for hepatocellular carcinoma. J Cancer Res Clin Oncol 2004;130:417−422.ArticlePubMedPDF
- 8. Singal A, Volk ML, Waljee A, Salgia R, Higgins P, Rogers MA, et al. Meta-analysis: surveillance with ultrasound for early-stage hepatocellular carcinoma in patients with cirrhosis. Aliment Pharmacol Ther 2009;30:37−47.ArticlePubMedPMC
- 9. Tzartzeva K, Obi J, Rich NE, Parikh ND, Marrero JA, Yopp A, et al. Surveillance imaging and alpha fetoprotein for early detection of hepatocellular carcinoma in patients with cirrhosis: a meta-analysis. Gastroenterology 2018;154:1706−1718. e1701.ArticlePubMedPMC
- 10. Colli A, Fraquelli M, Casazza G, Massironi S, Colucci A, Conte D, et al. Accuracy of ultrasonography, spiral CT, magnetic resonance, and alpha-fetoprotein in diagnosing hepatocellular carcinoma: a systematic review. Am J Gastroenterol 2006;101:513−523.ArticlePubMed
- 11. Kim SY, An J, Lim YS, Han S, Lee JY, Byun JH, et al. MRI with liver-specific contrast for surveillance of patients with cirrhosis at high risk of hepatocellular carcinoma. JAMA Oncol 2017;3:456−463.ArticlePubMedPMC
- 12. Yu NC, Chaudhari V, Raman SS, Lassman C, Tong MJ, Busuttil RW, et al. CT and MRI improve detection of hepatocellular carcinoma, compared with ultrasound alone, in patients with cirrhosis. Clin Gastroenterol Hepatol 2011;9:161−167.ArticlePubMed
- 13. Liu WC, Lim JH, Park CK, Kim MJ, Kim SH, Lee SJ, et al. Poor sensitivity of sonography in detection of hepatocellular carcinoma in advanced liver cirrhosis: accuracy of pretransplantation sonography in 118 patients. Eur Radiol 2003;13:1693−1698.ArticlePubMedPDF
- 14. Bennett GL, Krinsky GA, Abitbol RJ, Kim SY, Theise ND, Teperman LW. Sonographic detection of hepatocellular carcinoma and dysplastic nodules in cirrhosis: correlation of pretransplantation sonography and liver explant pathology in 200 patients. AJR Am J Roentgenol 2002;179:75−80.ArticlePubMed
- 15. Singal AG, Marrero JA, Yopp A. Screening process failures for hepatocellular carcinoma. J Natl Compr Canc Netw 2014;12:375−382.ArticlePubMedPMC
- 16. Choi JY, Lee JM, Sirlin CB. CT and MR imaging diagnosis and staging of hepatocellular carcinoma: part I. Development, growth, and spread: key pathologic and imaging aspects. Radiology 2014;272:635−654.ArticlePubMedPMC
- 17. Choi JY, Lee JM, Sirlin CB. CT and MR imaging diagnosis and staging of hepatocellular carcinoma: part II. Extracellular agents, hepatobiliary agents, and ancillary imaging features. Radiology 2014;273:30−50.ArticlePubMedPMC
- 18. Lee YJ, Lee JM, Lee JS, Lee HY, Park BH, Kim YH, et al. Hepatocellular carcinoma: diagnostic performance of multidetector CT and MR imaging-a systematic review and meta-analysis. Radiology 2015;275:97−109.ArticlePubMed
- 19. Marks RM, Ryan A, Heba ER, Tang A, Wolfson TJ, Gamst AC, et al. Diagnostic per-patient accuracy of an abbreviated hepatobiliary phase gadoxetic acid-enhanced MRI for hepatocellular carcinoma surveillance. AJR Am J Roentgenol 2015;204:527−535.ArticlePubMed
- 20. Tillman BG, Gorman JD, Hru JM, Lee MH, King MC, Sirlin CB, et al. Diagnostic per-lesion performance of a simulated gadoxetate disodium-enhanced abbreviated MRI protocol for hepatocellular carcinoma screening. Clin Radiol 2018;73:485−493.ArticlePubMed
- 21. Han S, Choi JI, Park MY, Choi MH, Rha SE, Lee YJ. The diagnostic performance of liver MRI without intravenous contrast for detecting hepatocellular carcinoma: A Case-Controlled Feasibility Study. Korean J Radiol 2018;19:568−577.ArticlePubMedPMC
- 22. Besa C, Lewis S, Pandharipande PV, Chhatwal J, Kamath A, Cooper N, et al. Hepatocellular carcinoma detection: diagnostic performance of a simulated abbreviated MRI protocol combining diffusion-weighted and T1-weighted imaging at the delayed phase post gadoxetic acid. Abdom Radiol (NY) 2017;42:179−190.ArticlePubMedPDF
- 23. Kim JS, Lee JK, Baek SY, Yun HI. Diagnostic performance of a minimized protocol of non-contrast MRI for hepatocellular carcinoma surveillance. Abdom Radiol (NY) 2020;45:211−219.ArticlePubMedPDF
- 24. Lee JY, Huo EJ, Weinstein S, Santos C, Monto A, Corvera CU, et al. Evaluation of an abbreviated screening MRI protocol for patients at risk for hepatocellular carcinoma. Abdom Radiol (NY) 2018;43:1627−1633.ArticlePubMedPMCPDF
- 25. Kim YK, Kim YK, Park HJ, Park MJ, Lee WJ, Choi D. Noncontrast MRI with diffusion-weighted imaging as the sole imaging modality for detecting liver malignancy in patients with high risk for hepatocellular carcinoma. Magn Reson Imaging 2014;32:610−618.ArticlePubMed
- 26. Kim HA, Kim KA, Choi JI, Lee JM, Lee CH, Kang TW, et al. Comparison of biannual ultrasonography and annual non-contrast liver magnetic resonance imaging as surveillance tools for hepatocellular carcinoma in patients with liver cirrhosis (MAGNUS-HCC): a study protocol. BMC Cancer 2017;17:877. ArticlePubMedPMCPDF
- 27. Ruggeri M. Hepatocellular carcinoma: cost-effectiveness of screening. A systematic review. Risk Manag Healthc Policy 2012;5:49−54.ArticlePubMedPMC
- 28. Cucchetti A, Trevisani F, Cescon M, Ercolani G, Farinati F, Poggio PD, et al. Cost-effectiveness of semi-annual surveillance for hepatocellular carcinoma in cirrhotic patients of the Italian Liver Cancer population. J Hepatol 2012;56:1089−1096.ArticlePubMed
- 29. Arguedas MR, Chen VK, Eloubeidi MA, Fallon MB. Screening for hepatocellular carcinoma in patients with hepatitis C cirrhosis: a cost-utility analysis. Am J Gastroenterol 2003;98:679−690.ArticlePubMed
- 30. Naimark D, Naglie G, Detsky AS. The meaning of life expectancy: what is a clinically significant gain? J Gen Intern Med 1994;9:702−707.ArticlePubMedPDF
- 31. Sarasin FP, Giostra E, Hadengue A. Cost-effectiveness of screening for detection of small hepatocellular carcinoma in western patients with Child-Pugh class A cirrhosis. Am J Med 1996;101:422−434.ArticlePubMed
- 32. Bruix J, Sherman M; American Association for the Study of Liver Diseases. Management of hepatocellular carcinoma: an update. Hepatology 2011;53:1020−1022.ArticlePubMedPMC
- 33. Kim HL, An J, Park JA, Park SH, Lim YS, Lee EK. Magnetic resonance imaging is cost‐effective for hepatocellular carcinoma surveillance in high‐risk patients with cirrhosis. Hepatology 2019;69:1599−1613.ArticlePubMed
- 34. Park SH, Kim B, Kim SY, Shim YS, Kim JH, Huh J, et al. Abbreviated MRI with optional multiphasic CT as an alternative to fullsequence MRI: LI-RADS validation in a HCC-screening cohort. Eur Radiol 2019;Dec 19 . doi: 10.1007/s00330-019-06546-5. [Epub ahead of print].ArticlePDF
- 35. Yang JD, Mannalithara A, Piscitello AJ, Kisiel JB, Gores GJ, Roberts LR, et al. Impact of surveillance for hepatocellular carcinoma on survival in patients with compensated cirrhosis. Hepatology 2018;68:78−88.ArticlePubMedPMC
References
Figure & Data
References
Citations

- Adding MRI as a Surveillance Test for Hepatocellular Carcinoma in Patients with Liver Cirrhosis Can Improve Prognosis
Su Jong Yu, Jeong-Ju Yoo, Dong Ho Lee, Su Jin Kim, Eun Ju Cho, Se Hyung Kim, Jeong-Hoon Lee, Yoon Jun Kim, Jeong Min Lee, Jae Young Lee, Jung-Hwan Yoon
Biomedicines.2023; 11(2): 382. CrossRef - MRI features of histologic subtypes of hepatocellular carcinoma: correlation with histologic, genetic, and molecular biologic classification
Ja Kyung Yoon, Jin-Young Choi, Hyungjin Rhee, Young Nyun Park
European Radiology.2022; 32(8): 5119. CrossRef - Imaging features of hepatobiliary MRI and the risk of hepatocellular carcinoma development
Jong-In Chang, Dong Hyun Sinn, Woo Kyoung Jeong, Jeong Ah Hwang, Ho Young Won, Kyunga Kim, Wonseok Kang, Geum-Youn Gwak, Yong-Han Paik, Moon Seok Choi, Joon Hyeok Lee, Kwang Cheol Koh, Seung-Woon Paik
Scandinavian Journal of Gastroenterology.2022; 57(12): 1470. CrossRef - Potential of a Non-Contrast-Enhanced Abbreviated MRI Screening Protocol (NC-AMRI) in High-Risk Patients under Surveillance for HCC
François Willemssen, Quido de Lussanet de la Sablonière, Daniel Bos, Jan IJzermans, Robert De Man, Roy Dwarkasing
Cancers.2022; 14(16): 3961. CrossRef - Prognosis of hepatocellular carcinoma patients diagnosed under regular surveillance: potential implications for surveillance goal
Joo Hye Song, Myung Ji Goh, Yewan Park, Joo Hyun Oh, Wonseok Kang, Dong Hyun Sinn, Geum-Youn Gwak, Yong-Han Paik, Moon Seok Choi, Joon Hyeok Lee, Kwang Cheol Koh, Seung Woon Paik
Scandinavian Journal of Gastroenterology.2021; 56(3): 274. CrossRef
 PubReader
PubReader ePub Link
ePub Link Download Citation
Download Citation
- Download Citation
- Close
- Related articles
-
- The efficacy of treatment for hepatocellular carcinoma in elderly patients
- Radiologic features of hepatocellular carcinoma related to prognosis
- Diagnostic performance of serum exosomal miRNA-720 in hepatocellular carcinoma
- Radioembolization for hepatocellular carcinoma: what clinicians need to know
- Liver transplantation for hepatocellular carcinoma with portal vein tumor thrombosis

 E-submission
E-submission THE KOREAN LIVER CANCER ASSOCIATION
THE KOREAN LIVER CANCER ASSOCIATION


 Follow JLC on Twitter
Follow JLC on Twitter